It starts like a regular cough, spreads easily at schools and grocery stores, and can threaten the lives of infants and newborns.
Pertussis, or whooping cough, is a vaccine-preventable disease now making a comeback in Canada, and most people who lived on Haida Gwaii in 2014 know it well.
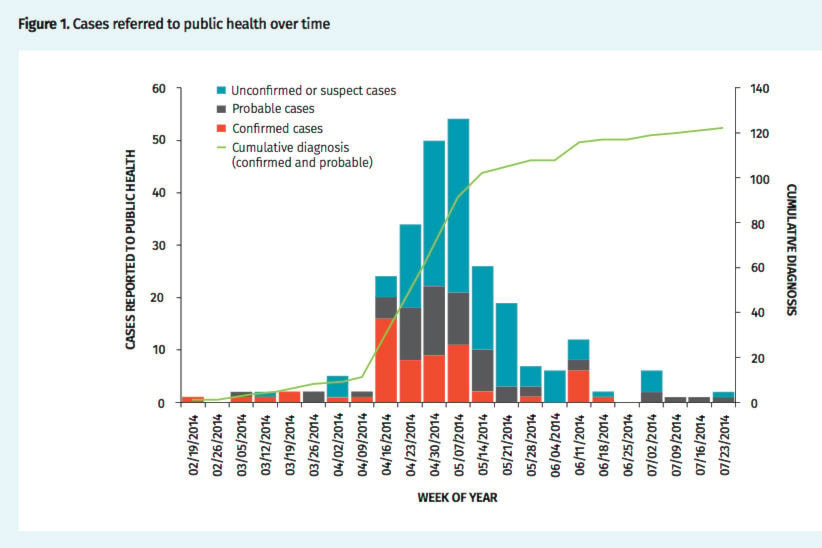
That year the islands endured a full-blown outbreak of the bacterial lung infection, with 123 confirmed and suspected cases from February to August.
“It had a little of the flavour of a disaster,” says Dr. Tracy Morton, a family physician in Queen Charlotte.
At one point, one in three kids at Sk’aadgaa Naay Elementary were infected. Six infants got it, and though all were fine, one needed two weeks in intensive care.
All told, doctors and nurses saw 579 people for pertussis-related care. Anyone treated with antibiotics had to stay home five days to stop the spread, effectively missing a week of work.
“It’s a big deal,” said Morton.
A study of the Haida Gwaii outbreak was published last month in Canadian Family Physician.
Morton led the study and hopes it shines a light on a key question for Haida Gwaii and other remote places — how and when should a disease outbreak be officially declared?
“Once an outbreak is declared, you get a heck of a lot more resources,” Morton explained.
For Haida Gwaii, the May 1 declaration kicked off an information campaign, better tracking of the outbreak’s spread, more aggressive testing and treatment.
Extra office staff and public health nurses were also sent over to help overloaded providers — nurses alone worked 400 overtime hours during the outbreak.
All that extra attention got results. Over 50 new pertussis patients came in the week after the outbreak was declared, and the number of new infections fell sharply after that.
But local providers had strongly suspected an outbreak long before May 1. By that time, they had seen 50 cases already.
Had they known what declaring an outbreak would mean, Morton said they would have called it much earlier.
Morton and his colleagues found several reasons for the delayed declaration, including a vacant medical health officer position at Northern Health.
In B.C., medical health officers are responsible for declaring outbreaks — a step that triggers an often costly and demanding response. Across Canada, each province sets its own criteria for when to declare one.
In California, where pertussis and other vaccine-preventable diseases are also resurgent, outbreaks are declared when the number of infected people reaches five times above normal.
The Haida Gwaii study recommended three big lessons for rural clinicians facing a similar disease outbreak: speak early with public health officials to track the spread of disease and to treat any women with a late-stage pregnancy; do not rely on lab testing to confirm cases because the results come far too slowly; and encourage universal childhood immunization.
Morton said a falling immunization rate is likely part of the reason pertussis is re-surging in Canada and the U.S. — a significant number of people have come to believe vaccines are somehow unsafe, despite evidence to the contrary. Although local statistics aren’t available, Haida Gwaii has several non-vaccinating families, though some changed their minds during the outbreak.
“What I can’t tell you is whether that stuck,” said Morton.
But for pertussis in particular, there is another problem.
Starting in 1996, every province in Canada began switching from using a more effective whole-cell pertussis vaccine to a partial-cell one that was less effective but also had fewer side effects.
Planners had seen pertussis rates fall from an average of 156 cases per 100,000 people before the vaccine was introduced in 1943 to a low of just five per 100,000 in the early 2000s.
Not only did pertussis look cornered, among all immunizations, the whole-cell pertussis vaccine happened to have the strongest possible side effects, including pain, fever, and even some febrile seizures in susceptible children.
So, as had been done with polio, planners moved to a less effective but also less challenging version of the pertussis vaccine.
“The hope was that this would be a more acceptable alternative,” Morton said.
“It’s only through the test of time that we’re getting a gradual but pretty steady rise in rates.”
The 2014 outbreak on Haida Gwaii was the most intense in the country that year, and Morton said it will likely contribute to an ongoing debate about how the pertussis vaccine schedule might need to change.
But most importantly, Morton and other local clinicians hope the experience encourages public health officials to set clear guidelines for when outbreaks get declared.
Pertussis usually follows a three- or four-year cycle, but just a year after the 2014 outbreak there was another cluster of pertussis infections on island.
Morton said the memory of the previous year’s outbreak was strong.
“We were super co-ordinated, we had public health here within the first week, communicating regularly,” he said.
“They didn’t declare it an outbreak, but boy did they deploy resources.”